The Levi laboratory is proud to present a publication in Nature Communications entitled “NGF-TrkA signaling dictates neural ingrowth and aberrant osteochondral differentiation after soft tissue trauma.”
Observations from developmental biology have previously clued in researchers into the possible link between nerves and bone formation. While the role for neurotrophic factors like Nerve Growth Factor (NGF) have been demonstrated to recapitulate patterns seen in developmental biology in the context of fracture and healing, the Levi Laboratory has demonstrated the importance of NGF in the regulation of post-traumatic heterotopic ossification, a manifestation of dysregulated inflammation and *aberrant* wound healing. New research recently published in the journal Nature Communications, describes a novel description of cellular programs that critically regulate and points to a possible new target for the mitigation of post-traumatic ectopic bone formation. The research team led by Dr. Benjamin Levi and Dr. Charles Hwang of the Department of Surgery’s section of plastic surgery, observed the effect of halting nerve transmission on HO. Using tissue from injury sites in mice that typically form HO, they demonstrated smooth muscle cells as being potent sources for NGF transcripts and also translated protein. Indeed, across multiple means of interfering with NGF activity by drugs or genetically prohibiting its production, post-traumatic heterotopic ossification was successfully attenuated. Denervation also precipitated changes within cell transcription, polarizing the typical TGFβ program to a FGF pattern, mitigating the terminal differentiation of these progenitor cells into cartilage and bone. Given the correlation with HO and pain, these investigators hope to translate these findings to patient therapies, inhibiting bone but also simultaneously mitigating the propagation of pain in patients with musculoskeletal polytrauma. This work exemplifies the invaluable cross-institutional collaboration with bony experts, Aaron W. James, Seungyong Lee, and Thomas Clemens, from Johns Hopkins University, along with the talented research teams throughout the laboratory. Special thank yous to the University of Michigan Department of Surgery and Section of Plastic Surgery, Center for Molecular Imaging, and the rest of the Levi laboratory team.
PMID: 34400627. (Read here!)
Abstract
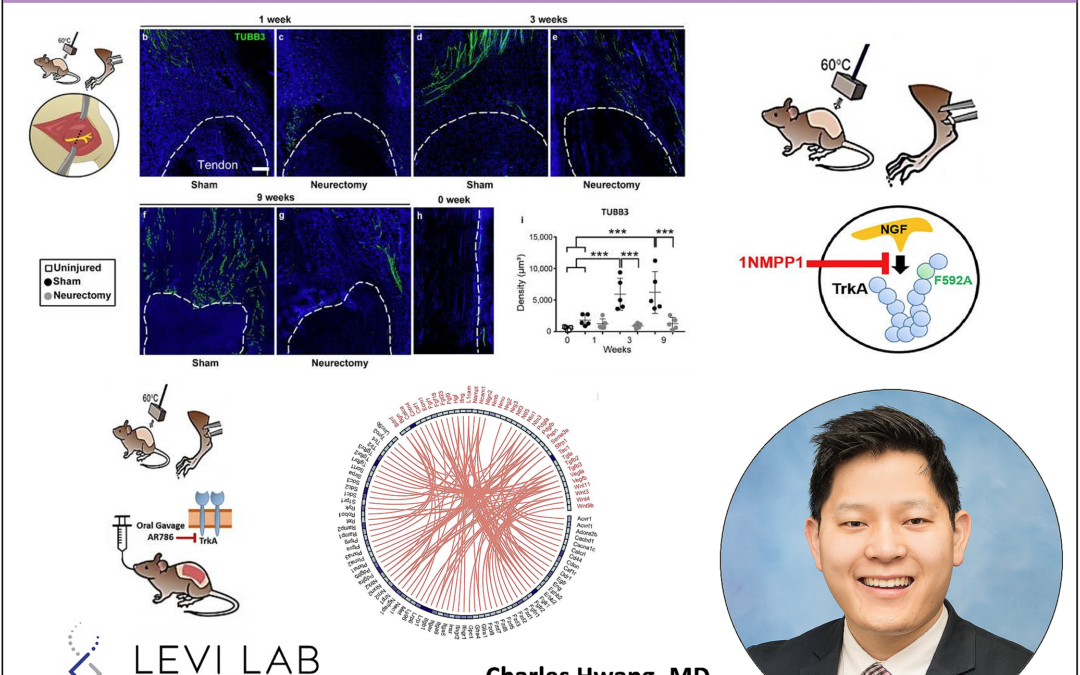
Pain is a central feature of soft tissue trauma, which under certain contexts, results in aberrant osteochondral differentiation of tissue-specific stem cells. Here, the role of sensory nerve fibers in this abnormal cell fate decision is investigated using a severe extremity injury model in mice. Soft tissue trauma results in NGF (Nerve growth factor) expression, particularly within perivascular cell types. Consequently, NGF-responsive axonal invasion occurs which precedes osteocartilaginous differentiation. Surgical denervation impedes axonal ingrowth, with significant delays in cartilage and bone formation. Likewise, either deletion of Ngf or two complementary methods to inhibit its receptor TrkA (Tropomyosin receptor kinase A) lead to similar delays in axonal invasion and osteochondral differentiation. Mechanistically, single-cell sequencing suggests a shift from TGFβ to FGF signaling activation among pre-chondrogenic cells after denervation. Finally, analysis of human pathologic specimens and databases confirms the relevance of NGF-TrkA signaling in human disease. In sum, NGF-mediated TrkA-expressing axonal ingrowth drives abnormal osteochondral differentiation after soft tissue trauma. NGF-TrkA signaling inhibition may have dual therapeutic use in soft tissue trauma, both as an analgesic and negative regulator of aberrant stem cell differentiation.